Psoriatic arthritis (PsA) is what is known as a ‘systemic’ condition, which means that it affects many body systems in addition to the joints. Not all the symptoms are joint-related.
The underlying inflammation that causes PsA also causes many of the symptoms outlined here. You may experience periods of time when your symptoms lessen or disappear altogether (remission) or when they ‘flare’ and become worse. Effective management of your PsA may help to treat the signs and symptoms below and keep them under control.
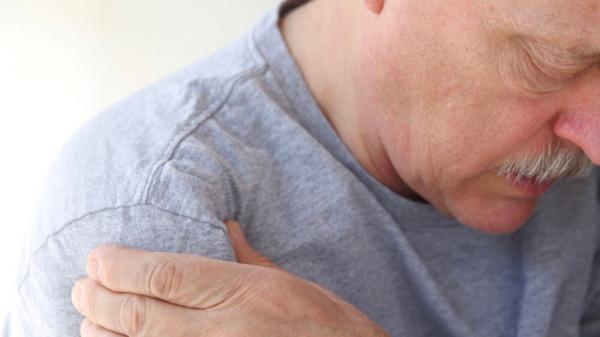
Swollen and painful joints
One of the key features of PsA is having one or more joints that are painful, stiff and, often, swollen. Any of the joints in the body can be affected but the joints most affected are the fingers, wrists, ankles and knees. Sometimes, the joints of the lower back or neck may also be affected. This is known as ‘spondylitis’. When the joints at the bottom of the spine just above the buttocks are affected, this is known as ‘sacroiliitis’. This joint pain and swelling are caused by the immune system mistakenly attacking the tissues in the joints.
The five patterns of joint pain
PsA often affects the body in certain patterns. These patterns have been categorised into five groups, although these patterns can overlap in the one individual:
- Asymmetric pattern: Between 1 and 3 joints are affected on different sides of the body, or ‘asymmetrically’. This is the mildest form of PsA.
- Symmetric pattern: The same joints are affected on both sides of the body with many more joints involved. This form of PsA looks a lot like rheumatoid arthritis.
- Distal pattern: The small joints in the fingers and toes closest to the nails are affected. This is often accompanied by distinctive changes to the nails themselves.
- Spinal pattern: This form of PsA affects the spine and may cause inflammation and stiffness in the neck, lower back, spinal, or pelvic area. This inflammation and stiffness can make movement difficult and painful.
- Destructive pattern: This form of PsA, also known as ‘arthritis mutilans’ is very rare. Like the distal pattern PsA, it primarily affects the small joints of the fingers and toes closest to the nails and can be severe. It is also often associated with lower back and neck pain. Early treatment is important to preserve function and reduce damage to the bones and joints.
Joint pain is can be one of the hardest parts of living with PsA. Understanding pain and learning techniques that may help you cope with pain are an important part of managing your PsA. Read the Dealing With Pain and the Joint Care resources for more information on ways to manage pain and look after your joints.
Fatigue
Fatigue is the medical term for the type of tiredness that disrupts your daily life and doesn’t get better after a good night’s sleep. It is one of the most common symptoms of PsA and is caused by the stress on your body when it is dealing with pain and inflammation.
There are a number of tips and strategies that you can develop to help deal with fatigue. Refer to the fatigue and arthritis resource for more information.
Psoriasis
Psoriasis is a condition that causes thick silvery scales (known as plaques), or dry red patches of skin to form. These patches are often itchy and may also be painful. Psoriasis can occur anywhere on the body and may appear in hard to see areas like on the scalp, in the navel (belly button) or between the buttocks.
Most people with PsA also have psoriasis. Mostly the diagnosis of psoriasis comes before that of PsA but some people develop PsA first. There are also some people who never develop the skin disease. For these people, a family history of psoriasis or PsA is required for a diagnosis.
PsA may be more common in people with more severe skin disease, but the severity of the skin and joint disease are not linked. This means that people with severe psoriasis may develop minor arthritis symptoms and vice versa.
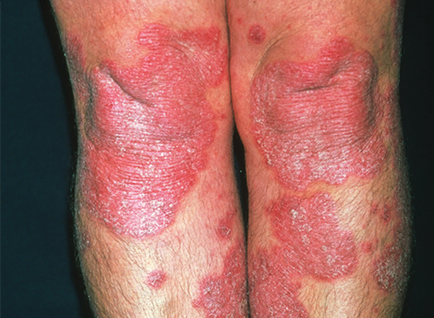
Image appears with permission from getpsorted
Enthesitis
Enthesitis is inflammation of the ‘entheses’, the places in the body where the tendons or ligaments attach to the bones. This usually causes pain at the affected site that gets worse with movement. Stiffness in the nearby joints is also common. Pain and swelling on the back of the heel is very common in people with PsA and is caused by enthesitis of the Achilles tendon.
Please refer to the Enthesitis in psoriatic arthritis resource for more information.
Dactylitis
Dactylitis is inflammation of the small joints of the fingers and/or toes (the digits) and of the entheses of the surrounding tendons. It is sometimes referred to as ‘sausage digits’ because the whole of the finger or toe becomes swollen, making it painful and hard to bend.
Around 40% of people with PsA will experience dactylitis. The joints in the toes are almost twice as likely to be affected as the fingers.
Swollen digits are also common in other forms of arthritis, such as rheumatoid arthritis, but the pattern of joints affected is different in PsA. For example, in rheumatoid arthritis the same joint is typically affected on several digits in a ‘ray’ pattern. In contrast, all three joints in one digit tend to be affected in PsA.
For these reasons, dactylitis is often used to help distinguish PsA from rheumatoid arthritis.
Changes to the fingernails or toenails
Another sign of PsA may be changes to the look and structure of the nails on the fingers or toes. These changes are related to psoriasis and may be called ‘nail psoriasis’. Around 40% of people with skin psoriasis alone will have some nail symptoms. Up to 80% of people with PsA will experience these symptoms.
Pitting of the nails (small shallow dents in the nails) is the most common symptom in people with PsA. It is caused by inflammation of the tissue that causes nail growth. Nail pitting also occurs in other conditions, such as eczema, but the pits are often deeper in people with psoriasis and PsA.
Another common change to the nails in people with PsA is when the nail lifts away from the nail bed underneath. This usually starts at the tip of the nail (known as onycholysis). The space created by this lifting away can increase the risk of infections, making good hand hygiene more important than usual.
In addition to changing the look of the nails, nail psoriasis can also cause pain and discomfort and can affect daily living activities and mental wellbeing.
Image appears with permission from VisualDx/Skinsight
Uveitis
Uveitis is an inflammation of the middle layer of the eye (the uvea). The most common form of uveitis is iritis, an inflammation of the iris at the front of the eye. It is also known as ‘anterior uveitis’.
Symptoms include pain and redness of the eye, watery eyes, blurry vision and sensitivity to light. Symptoms can occur in just one eye or may occur in both at the same time.
Uveitis affects up to one in four people with PsA. Uveitis is more common in people who smoke.
Please refer to the Uveitis in psoriatic arthritis resource for more information.
This is not a complete list of all the possible symptoms of PsA. You may experience symptoms that are not covered here. Discuss possible symptoms or anything you are concerned about with your doctor.
This resources has been developed based on the best available evidence. A full list of resources is available on request.